What is hemifacial spasm?
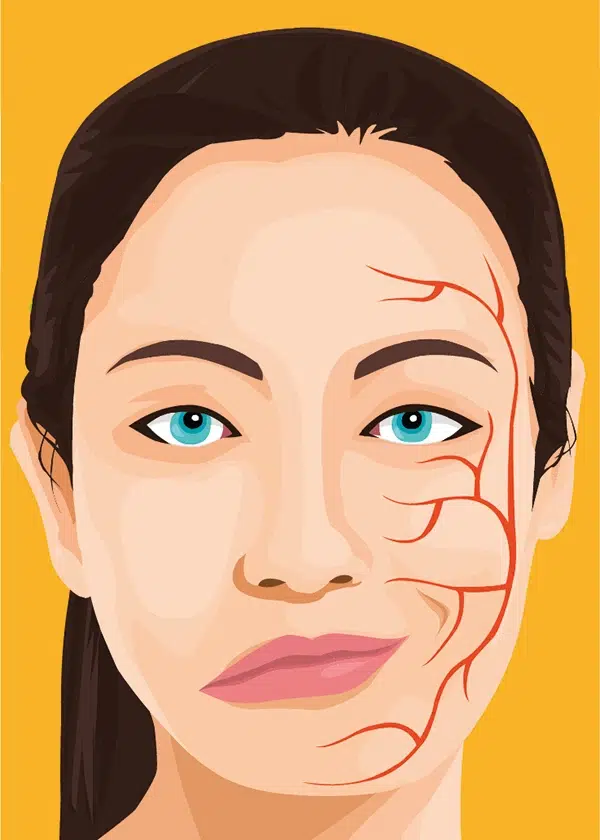
Hemifacial spasm (HFS, also known as tic-convulsive) is an uncontrolled twitching of the facial muscles, usually one side of the face.
What are mimetic muscles and how they are controlled?
There are about 600 muscles in human body. Most of them are deep and attach to bones. Muscles are capable of contraction and by doing so they move the bones. Facial muscles (AKA mimetic muscles) are different. Firstly they are located shallow, directly under the skin. Secondly, they originate from the skull and terminate in the skin of the face. Their contractions therefore moves the skin of the face. Facial muscles are extremely important for speaking, eating, blinking and facial expressions during communications. All emotions that we experience are reflected in our face by facial muscles. Therefore, they also known as mimetic muscles. Facial muscles are also responsible for wrinkling which is basically is a skin fold that develops over particular muscle and is always perpendicular to the line of contraction.
What is the facial nerve and what does it do?
All mimetic muscles are innervated by the facial nerve (VII cranial nerve). The facial nerve is predominantly a motor nerve and mostly it contains fibers designated to mimetic muscles. Like any other cranial motor nerve, its nucleus located deep in the brainstem. Nucleus is basically a congregation of neurons performing a specific function. Facial nucleus neurons are responsible for taking orders from the brain cortex and delivering it to facial muscles. Each neuron has a single, very long protrusion called axon. Axon is the cellular structure connecting the neuron to the muscle. It is basically a communication line between the neuron and the muscle fibers. The communication is one way i.e. neuron generates electric impulses which travel along the axon to the muscle fibers. Once the impulse reach muscle fibers they respond by contracting. When muscles do not receive impulses it does not contract i.e. in the idle mode.
Myelin
Axons are wrapped with specific cells that nurture them and speed up impulse velocity. In the brain this coating is provided by oligodendrocytes and outside of the brain by Schwann cells. They contain a very specific substance called myelin. Myelin is very important for speedy impulse propagation. Additionally, myelin provides insulation for axons. Axons plus supportive cells with myelin are called nerve fibers. Nerve fibers from all facial neurons assemble, leave the brainstem and travel to the facial muscles. This cluster of nerve fibers is known as the facial nerve.
The facial nerve
Any nerve is like a cable containing a lot of individual nerve fibers and the facial nerve is no different. It contains thousands of fibers1. Each nerve fiber is operating independently i.e. under normal conditions impulses between different fibers don’t mingle with each other. This feature is essential for orderly contraction of the muscles. The main structure maintaining this independence is myelin. It is a very good insulator and therefore electric impulses from one fiber do not jump to the other.
The facial nerve enters the temporal bone through internal auditory canal and then passes through the specific canal inside the bone called facial canal. It receives sensory and parasympathetic fiber on its way. After leaving the skull just under the ear facial nerve branches off. These individual branches reach mimetic muscles and make them contract upon stimulation.
How does hemifacial spasm develop?
Movement disorders
As mentioned previously coordinated contraction of the muscles is very important for proper function. One of the most important features of muscle contraction is voluntary control. We can control our facial expressions as well any other muscle in our body.
There are several diseases when muscles contract involuntary (i.e. out of our control) which are collectively called movement disorders. These movements are non-functional i.e. do not have a purpose. Hemifacial spasm is one of movement disorders. Unlike other diseases in this category it is well-understood and is treatable.
Root entry exit zone
Hemifacial spasm is the disease of the facial nerve. Specifically, the condition develops at the point of nerve’s exit from the brainstem. This area is called root-entry-exit-zone or simply REEZ. One of the interesting points about REEZ, is the transition from central myelin to peripheral. As discussed above, myelin is an insulating coating provided by specific cells – oligodendrocytes in the brain and Schwann cells outside. Oligodendrocytes meet Schwann cells in the REEZ area. This is a transitional zone where nerve fibers lack myelin and vulnerable to excitation.
The dominant theory regarding origin of hemifacial spasm assumes that there is cross-spread of neural impulses in the REEZ. In other words, normal impulses passing via nerve fibers spread to other, idle fibers and cause their excitation. Normally, myelin acts like an insulator and blocks sideways cross fiber excitation. However, if myelin is deficient there might be cross-excitation between the fibers. These abnormal impulses propagate distally, reach unrelated muscles and cause involuntary contractions. For example, fibers innervating lip and eyelid muscles are different and under normal circumstances operate independently. However, if excitation of lip fibers spreads to eyelid fibers eyelid muscles will contract (blink) each time the patient talks. Synkinesis is a medical term describing this phenomenon and it is typical in hemifacial spasm patients.
Ephaptic transmission and ectopic activation
Under normal conditions every fiber has minimal activity i.e., number of impulses per second is very low. This baseline activity maintain normal muscle tone. When muscle activation is required fibers fire up. In other words number of impulses increase. As discussed above every fiber is operating independently and there is no cross talk between fibers. In hemifacial spasm patients impulses jump from activated fibers to unactivated ones. Usually the involuntary activity spreads to the most of facial nerve fibers and causes twitching of the half of the face (here is the name – hemifacial spasm). Such “lateral” or “ephaptic” transmission is the main mechanism contributing to disease progression. The greater the compression at REEZ area the higher cross talk rate between fibers and the worse the clinical situation. Ephaptic transmission is responsible for synkinesis and activity induced hemifacial spasm.
Cross-excitation is not the sole factor contributing to hemifacial spasm. With time an abnormal ectopic excitation zone may develop in the facial nerve. This focus does not need normal impulses to maintain activity and may self generate abnormal impulses on its own. At this stage the patients usually have facial spasms independently from activation.
What are the causes of hemifacial spasms?
Hemifacial spasm is quite rare with prevalence 8-10 cases per 100,000 people2. As discussed above REEZ is a sensitive area with a potential for transformation into a ectopic site. But it usually does not because the transition zone is very short and myelin sufficiently insulates individual fibers.
In order to develop hemifacial spasm there must be an additional damaging factor in the REEZ area. This damaging factor should result in loss in myelin (demyelination). Depending of the causes, HFS can be classified as primary or secondary. Primary or idiopathic hemifacial spasm develops independently of other diseases and is the most common form. Secondary HFS is a consequence or by-product of other conditions.
Neuro-vascular conflict
This form is the most frequent one and is also known as primary or idiopathic. Compression of the facial nerve by a blood vessel is the main pathophysiological mechanism. Usually, anterior inferior cerebellar artery (AICA) exerts pressure on the facial nerve due to natural proximity. Occasionally, distant arteries like posterior inferior cerebellar artery (PICA) or vertebral artery (VA) may be dolichoectatic (excessively long and wide) and deviate from natural course toward the facial nerve. Venous as well as multiple vessel compression may produce neuro-vascular conflict as well.
Typically a loop of offending vessel pushes and distorts the facial nerve at the brainstem. Sometimes collision is very severe resulting in nerve flattening. A vascular loop buried into the nerve is not uncommon. Arterial compression is most severe due to two factors. First, arterial blood pressure is higher than venous generating greater compressing force. Second, arteries pulsate and hit the nerve like a hammer with every heart beat. Neuro-vascular conflict is progressive i.e. arterial loops exert more and more pressure on the nerve with aging.
Familial hemifacial spasm
Most cases of hemifacial spasm are idiopathic and caused by neuro-vascular conflict. However, there have been reports in the literature describing hereditary HFS cases3. In this situations close relatives seem to have hemifacial spasms. The exact genetic mechanism underlying familial HFS is unknown but it looks like that there is autosomal dominant with low penetrance inheritance pattern. Strangely, familial cases have remarkable 90% left side predominance while idiopathic cases are equally right and left sided.
Bell’s palsy
Facial palsy in some sense is opposite of hemifacial spasm. Bell’s palsy is the inflammation of the facial nerve with resultant impairment of impulse propagation. As a consequence, mimetic muscles do not receive impulses and become paralyzed. Most facial palsies improve and the patients resume their normal or near normal facial features. Recovery includes re-growth of individual neural fibers and mismatches are not uncommon. Axons may regenerate along a wrong path. For example, fibers designated for lip muscles may end up in eyelid muscles. As a result, patients may develop synkinesis – an involuntary, synchronous twitching evoked by a normal movement. For example, speaking may induce eye blinking. Synkinesis are usually mild after Bell’s palsy and most patients do not progress to hemifacial spasm. Ectopic zones may develop in minority facial palsy patients during recovery and lead to HFS .
Tumor
Sometimes tumors in close proximity of the facial nerve may trigger HFS. However, tumors do not pulsate (not as much as arteries), grow slowly and allow adaptation. Therefore, hemifacial spasm in the presence of tumor is quite rare though certainly possible.
Arachnoid cyst
These are fluid filled cavities in the subarachnoid space. They are quite common but rarely cause problems. Yet, sometimes they may grow big and compress the cranial nerves. Sometimes the facial nerve may get displaced by arachnoid cyst and pushed toward an artery that it wouldn’t otherwise touch. In these cases the facial nerve is literally smashed between the cyst and artery.
Epidermoid tumor or cyst
Epidermoid cysts are benign tumors frequently seen in around facial nerve. They do not have blood vessels, grow slowly and are simply epidermal inclusions in the brain. Sometimes they may be complex and contain hair or teeth. Like tumors they may compress the facial nerve and induce hemifacial spasm.
Multiple sclerosis (MS)
MS is a debilitating neurological disease characterized by loss of myelin coating of the nerve fibers in the brain. Typically the patients develop multiple sclerosis plaques in various brain areas. If there is demyelination in the facial nerve there is a chance of developing hemifacial spasm. Unlike other causes, this type of HFS cannot be treated surgically. Only treatment of the main disease i.e. MS itself can provide relief. It should be noted that other demyelinating diseases can cause hemifacial spasm as well. For example, AIDS can cause loss of myelin and consequently lead to hemifacial spasm.
Hemifacial spasm is very similar to trigeminal neuralgia (TN). These diseases have much in common, the only difference is the affected nerve. Trigeminal nerve (V cranial nerve) is implicated in TN and the main symptom is facial pain.
How is hemifacial spasm (HFS) diagnosed?
Clinical examination
The diagnosis of hemifacial spasm is pretty straightforward for an experienced clinician. The half of the face has irregular, uncontrolled contractions that are usually triggered by speech, laughter, or emotional expressions. The appearance of spasms is typical and unforgettable. Twitching is clonic and so typical that no other methods are necessary to make the diagnosis. One of the unique signs observed only in HFS is Babinski 2 sign ( AKA “the other” Babinski sign or “brow-lift sign”)4 . It constitutes simultaneous elevation of the eyebrow and closure of the eye and is pathognomonic for hemifacial spasm. Another characteristic feature of hemifacial spasm is nocturnal spasms. The twitching does not stop at night i.e. during sleep. This feature helps to differentiate HFS from psychogenic hemifacial spasm. Occasionally, there might be atypical clinical presentation and diagnosis might not be so obvious.
Functional blindness
In addition to muscle twitching hemifacial spasm may cause several physical signs. In severe hemifacial spasm cases, persistent contractions of periorbital muscles cause constant eye closure. As a result, patients develop functional blindness which may significantly lower patients’ quality of life.
Dry eye syndrome
Hemifacial spasm is caused by focal demyelination of the facial nerve at the brainstem level. Parasympathetic fibers responsible for normal lacrimation are passing inside the facial nerve and may be damaged by neuro-vascular conflict. This damage is the main mechanism leading to dry eye syndrome which later may cause corneal damage and lead to permanent visual loss.
Bilateral hemifacial spasm
Hemifacial spasm affects one half of the face in the majority of cases. However, both sides can be affected. Usually spasms start on one side and then progressively spread to the other one. Bilateral hemifacial spasms may present serious diagnostic challenges. Many clinicians are unaware of this clinical variant and attribute full face involvement to different movement disorders.
Hemifacial spasm in combination with facial palsy
In some cases, the facial nerve may be overly compressed and stretched, resulting in partial facial palsy. In fact, any demyelination in the facial nerve leads to subtile palsy but it is rarely noticeable. Occasionally facial palsy might be discernible. Such combination of facial palsy and spasms may be perplexing for inexperienced physicians. Obviously, secondary HFS developing as a consequence of Bell’s palsy will also include residual facial palsy. Focusing on the history of Bell’s palsy physicians may fail to recognize hemifacial spasm and wrongly attribute twitching to neurogenic sequela of the Bell’s palsy. Mixture of facial palsy and spasms is typical in patients who had previous Botox injections.
Tonic (sustained) hemifacial spasm
A typical feature of hemifacial spasms is clonic twitching of the facial muscles. In rare cases, the condition is extremely severe and compression locks all mimetic muscles in a state of sustained contraction without twitching. These prolonged episodes are puzzling and may cause diagnostic problems. Physicians may misdiagnose tonic hemifacial spasm with Bell’s palsy of the unaffected side and even proceed with treatment.
Hearing abnormalities
Hemifacial spasm is the movement disease of the facial muslces. However, there are several auditory abnormalities frequently accompanying HFS. Usually, the patients experience mild hypoacusis (hearing loss), ear clicks or tinnitus. The exact mechanism of HFS associated acoustic phenomena is unknown. There are several plausible theories to explain clinical observations5.
- Stapedius muscle spasm. Stapedius muscle is the smallest muscle in human body. It is attached to the stapes bone (which happens to be the smallest bone in human body). Its main function is to stabilize stapes bone and prevent excessive vibrations. Stapedius muscle receives innervation from facial nerve branch and facial nerve diseases affect stapedius muscle. For example in Bell’s palsy stapedius muscle becomes paralyzed which results in hyperacusis syndrome. In hemifacial spasm, the situation is the opposite. Abnormal impulses may induce aberrant muscle contractions which in turn may interfere with sound transmission and cause hypoacusis.
- Concomitant cochlear nerve compression. Anatomically, the facial nerve (VII nerve) is very close to the VIII cranial nerve – vestibulo-cochlear nerve. Cochlear nerve conducts hearing impulses from the inner ear. The 7th nerve is so close to 8th that a vessel compressing the facial nerve may compromise the cochlear nerve as well and cause hearing abnormalities.
- Eustachian tube (ET) dysfunction. ET is tiny channel connecting the nasopharynx with the middle ear. Abnormal facial contractions may interfere with Eustachian tube’s function and cause ear clicks. However, it is not clear how facial muscles may influence Eustachian tube because none of them is directly related to the ET.
Imaging studies
Imaging studies are essential part of the diagnostic process. The most frequent type of HFS is idiopathic one due to neuro-vascular conflict. MRI is usually capable of demonstrating this compression if properly obtained. However, that standard brain MRI usually misses this condition. Only specialized sequences like Constructive Interference Steady State (CISS) and Fast Imaging Employing Steady State Acquisition (FIESTA) are capable of showing intricate anatomy of the facial nerve and its surroundings. These specific, ultra thin, high resolution scans nicely visualize the neuro-vascular conflict (or lack of thereof).
In the vast majority of case the offending vessel is anterior inferior cerebellar artery (AICA). It is a branch of vertebral artery and provides blood supply to the parts of brainstem and cerebellum. Occasionally, normally sized AICA makes a loop around facial nerve and compresses it at the brainstem exit point. Other brain arteries that can cause compression are posterior inferior cerebellar artery (PICA) or vertebral artery. Normally these arteries are far away from the facial nerve but in exceptional cases they are dolichoectatic i.e., elongate, enlarge and make abnormally long loops. These cases are very explicit and can be easily recognizeble on MRI scans.
In cases of secondary HFS MRI may explicitly diagnose tumors, arachnoid cysts, epidermoid cysts, demyelination as a cause of hemifacial spasm.
Electromyography
EMG is a very useful tool in hemifacal spasm. There are several pathognomonic EMG signs that can make substantial contributions the diagnosis. EMG may show cross-talk between fibers and rule out other movement disorders6. Yet, in practice many physicians do not routinely use EMG due to characteristic presentation and reserve it for atypical cases.
Differential diagnosis
There are many diseases that mimic hemifacial spasm7.
- Psychogenic hemifacial spasm
- Facial Tics
- Facial Myoclonus
- Oromandibular Dystonia
- Hemimasticatory Spasm
- Blepharospasm
- Facial myokymia
Next: Hemifacial Spasm Treatment
References
- Thurner KH, Egg G, Spoendlin H, Schrott-Fischer A. A quantitative study of nerve fibers in the human facial nerve. Eur Arch Otorhinolaryngol. 1993;250(3): 161-167. https://doi.org/10.1007/BF00171704 [↩]
- Nurminen P, Marjamaa J, Niemela M, Sairanen T. Incidence and prevalence of Hemifacial Spasm in Finland’s largest hospital district. J Neurol Sci. 2023;446: 120587. https://doi.org/10.1016/j.jns.2023.120587 [↩]
- Miwa H, Mizuno Y, Kondo T. Familial hemifacial spasm: report of cases and review of literature. J Neurol Sci.2002;193(2): 97-102. https://doi.org/10.1016/s0022-510x(01)00651-7 [↩]
- Varanda S, Rocha S, Rodrigues M, Machado A, Carneiro G. Role of the “other Babinski sign” in hyperkinetic facial disorders. J Neurol Sci. 2017;378: 36-37. https://doi.org/10.1016/j.jns.2017.04.036 [↩]
- Rudzinska M, Wojcik M, Zajdel K, et al. The influence of botulinum toxin on auditory disturbances in hemifacial spasm. Neurol Neurochir Pol. 2012;46(1): 29-36. https://doi.org/10.5114/ninp.2012.27451 [↩]
- Lefaucheur JP, Ben Daamer N, Sangla S, Le Guerinel C. Diagnosis of primary hemifacial spasm. Neurochirurgie. 2018;64(2): 82-86. https://doi.org/10.1016/j.neuchi.2017.12.003 [↩]
- Yaltho TC, Jankovic J. The many faces of hemifacial spasm: differential diagnosis of unilateral facial spasms. Mov Disord. 2011;26(9): 1582-1592. https://doi.org/10.1002/mds.23692 [↩]